Yoga Pose
Posted on June 16, 2021 by Rebecca Seto-Leung
Did you know that cat cow poses and Child’s pose can help stretch out your lower back? Stretching can help improve flexibility and lengthen the muscles that have been shortened over time. Strengthening the core muscles with plank poses and mini crunches along with glutes bridges can also help. Does a registered massage therapy treatment to relieve tension in the lower back sound good to you? We’re here to support you! Book in with us at ruperthealth.com
Meditation
Posted on June 12, 2021 by Rebecca Seto-Leung
Let’s take a moment to pause, be still and assess where we are at with our mind. The emphasis may be on how the body feels but let’s not forget the connection between the body and mind. One way to meditate is to reflect on this question, “what are you most grateful for in your life at this moment?” Thinking about all the things that you are grateful for or what is going well in your life allows you to create a feeling of appreciation of life that can overflow into your relationships with others and into your journey through life. At Rupert Health we are grateful to all of our patients, we are thankful that during a pandemic we can still assist you with safety measures in place and we appreciate your trust and support in us. Whether it is registered massage therapy, chiropractic care or exercise rehabilitation, we are here to support you, always. Your appointment is ready for you at ruperthealth.com
Relaxation during work
Posted on June 11, 2021 by Rebecca Seto-Leung
Time to step away from your desk, your work will be there when you get back. Stand with your feet hip width apart, bring your hands together behind you, put one thumb on top of the other and bring your shoulders back and down. Take an inhale in and a long exhales out, relax your shoulders down. Twice more, big inhale in and long exhale out. Switch hands and use other thumb this time, bring your shoulders back and down. Again, with two deep inhales in and long exhales out. Feel free to add slow neck circles, nodding “yes” then “no”. Does a registered massage therapy treatment focusing on your middle of the back, shoulders, arms and neck with strengthening to retract your shoulders back sound good to you? Your appointment is ready for you at ruperthealth.com
Type of Rest that Every Person Needs
Posted on June 9, 2021 by Rebecca Seto-Leung
A recent TED Talk discusses the “7 types of rest that every person needs.” The first type, physical rest can be active or passive. Passive rest is achieved by sleeping and napping while active rest obtained by ways including yoga, stretching and massage therapy. Yoga and stretching may improve one’s flexibility while massage therapy has been shown to improve one’s circulation, decrease blood pressure and reduce heart rate. Is getting more rest your self-care goal for the New Year? We’re here to support you, book your registered massage therapy appointment at ruperthealth.com
Bell’s Palsy
Posted on June 5, 2021 by George Wang
What is Bell’s Palsy ?
Bell’s palsy is a condition that includes rapid weakness in facial muscles. For most cases, the condition is temporary and improved over weeks. The weakness of facial muscle causes half of patient’s face appears to drop, one sided smile and inability to close the eye from that side.
Bell’s palsy is also known as acute peripheral facial palsy. The exact cause of weakness in facial muscle is still unknown, but it can occur at all ages. However, it is believed that the weakness is caused by following two. One could be the result of inflammation of the seventh cranial nerve, which carries electrical signals between the brain and facial muscles. The other one could be a reaction of viral infection.
Bell’s palsy is temporary for most cases. Usually within weeks, the muscle weakness will start to improve and completely recover in half of a year.
Symptoms
Rapid onset of mild weakness to total paralysis on one side of the face
Facial droop and difficulty to make facial expression, such as closing eyes or smiling
Drooling
Pain around the jaw or in or behind the ears on the affected side
Increased sensitivity to sound on the affected side
Headache
Loss of taste
Changes in the amount of tears and saliva you produce
See A Doctor
See a doctor when you experience any type of paralysis because you may have a stroke. Although Bell’s palsy is not caused by a stroke, the symptoms are similar. Typically, most cases recover fully with or without treatment and surgery is rarely an option for Bell’s palsy. Go to visit your GP when you experience facial weakness or drooping to seek underlying causes and severity of the illness.
Citation
Mayo Foundation for Medical Education and Research. (2020, April 2). Bell’s palsy. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/bells-palsy/symptoms-causes/syc-20370028.
Cause of Different Types of Back Pain
Posted on February 10, 2021 by George Wang
Lower back pain is common among population. Prior to treatment by health care professionals, it is useful to have an understanding on different diagnostic categories of lumbar discs terminology.
Normal
Defines discs that are morphologically normal, without the consideration of the clinical context and not inclusive of degenerative, developmental, or adaptive changes that could be considered clinically normal (Fardon, Williams, Dohring, Murtagh, Rothman & Sze, 2014, p.3).
Congenital/developmental variation
Includes discs that are congenitally abnormal or that have undergone changes in their morphology as an adaptation of abnormal growth of the spine, such as from scoliosis or spondylolisthesis (Fardon, Williams, Dohring, Murtagh, Rothman & Sze, 2014, p.3).
Degeneration
Includes subcategories of annular fissure, degeneration, and herniation
Annular fissure refers to separations between the annular fibers or separation of annular fibers from their attachments to the vertebral bone (Fardon, Williams, Dohring, Murtagh, Rothman & Sze, 2014, p.3).
Degeneration refers to all of the following: desiccation, fibrosis, narrowing of the disc space, diffuse bulging of the annulus beyond the dis space, fissuring, mucinous degeneration of the annulus, intradiscal gas, osteophytes of the vertebrae apophyses, defects, inflammatory changes, and sclerosis of the end plates (Fardon, Williams, Dohring, Murtagh, Rothman & Sze, 2014, p.4)
Herniation refers to a localized r focal displacement f disc material beyond the limits of the intervertebral disc space. The disc material may be nucleus, cartilage, fragmented apophyseal bone, annular tissue, or any combination thereof (Fardon, Williams, Dohring, Murtagh, Rothman & Sze, 2014, p.4).
Herniated disc may be classified as protrusion or extrusion, contained or uncontained (Fardon, Williams, Dohring, Murtagh, Rothman & Sze, 2014, p.5-6).
- Protrusion is present if the greatest distance between the edges of the dis material presenting outside the disc space is less than the distance between the edges of the base of that disc material extending outside the disc space
- Extrusion is present when, in at least one plane, any one distance between the edges of disc material beyond the disc space is greater than the distance between the edges of the base of the disc materials beyond the disc space or when no continuity exists beyond the disc space and that within the disc space
- Contained refers to if the displaced portion is covered by outer annulus fibers and/or the posterior longitudinal ligament;
- Uncontained when absent of such covering
Trauma
Includes disruption of the disc associated with physical and/or imaging evidence of violent fracture and/or dislocation and does not include repetitive injury, contribution of less than violent trauma to the degenerative process, fragmentation of the ring apophysis in conjunction with disc herniation, or disc abnormalities in association with degenerative subluxations (Fardon, Williams, Dohring, Murtagh, Rothman & Sze, 2014, p.6-7).
Inflammation/infection
Includes infections, infection-like inflammatory discitis, and inflammatory response to spondyloarthropathy. Includes inflammatory spondylitis of subchondral end plate and bone marrow manifested by Modic Type I MRI changes and usually associated with degenerative pathological changes in the discs (Fardon, Williams, Dohring, Murtagh, Rothman & Sze, 2014, p.7).
Neoplasia
Refer to primary or metastatic morphologic changes of disc tissues caused by malignancy (Fardon, Williams, Dohring, Murtagh, Rothman & Sze, 2014, p.7).
Miscellaneous paradiscal masses of uncertain origin
Refer to a paradiscal mass or an increase in the size of herniated disc material may be created by epidural bleeding and/or edema, unrelated to trauma or other known origin (Fardon, Williams, Dohring, Murtagh, Rothman & Sze, 2014, p.7).
Citation
Fardon, D. F., Williams, A. L., Dohring, E. J., Murtagh, F. R., Gabriel Rotheman, S. L., & Sze, G. K. (n.d.). Lumbar disc nomenclature: Version 2.0 Recommendations of the combined task forces of the North American Spine Society, the American Society of Spine Radiology and the American Society of Neuroradiology. The Spine Journal. doi:https://doi.org/10.1016/j.spinee.2014.04.022
Link to the article: https://ruperthealth.com/research/lumbardisc.pdf
Mindfulness and Stress Reduction
Posted on December 27, 2020 by admin
The physical results of stress:
Stress can have a negative impact on our physical health and cause things such as headaches, stiffness, muscle aches, and pains. Additionally, tight muscles can lead to posture issues and poor sleep, which can end up creating more stress.
To avoid stress affecting your physical health, make sure to always adjust your posture especially at times when you are feeling stressed. Having improper posture frequently can lead to problems with your back and spine overtime. If you are clenched up and feeling stressed, check your posture and adjust your posture so that you are sitting up tall and straight. To make sure you are maintaining a straight back position, it is best to sit on a chair with back support or have your back against a wall.
The importance of mindfulness:
Mindfulness meditation is a common technique used to combat stress, anxiety, chronic pain, depression, and headaches. Add mindfulness to your everyday routine; even as little as 10 minutes can make a big difference in our overall sense of well-being. Meditation is easy to implement to anyone’s lifestyle, as it is a cost saving practice that involves low physical and emotional risk and has the potential to empower people to be more actively engaged in their mental health.
Some significant health benefits of mindfulness are insignificant improvements in pain, anxiety, overall well-being, and the ability to participate in daily activities. Incorporating mindfulness frequently has also been found to improve your overall mood and reduce stress.
Ways to practice mindfulness:
Workspace Ergonomics
Posted on December 2, 2020 by admin
What is Ergonomics?
Ergonomics is the science of fitting workplace conditions and job demands to workers’ capabilities. For example, the size data of human bodies to design chairs, tables, and walkways. While many people are adjusting to working from home, it is important to create an environment that is ergonomically friendly, especially for those who are sitting at a desk for long periods of time. Creating a proper ergonomic workspace is crucial to keep you comfortable at work and can prevent injuries from occurring overtime.
Creating the Perfect Ergonomic Workspace
Consider following these tips when creating a suitable workspace:
1. Choosing the right chair
- Adjust your chair’s height to make sure that your feet rest flat on the ground. Make sure that your hips, feet and elbows are bent at 90 degrees. Use a footrest to support your feet if needed. Armrests of your chair should be adjusted so that your arms can rest on them with ease, ensuring that your neck and shoulders are relaxed downwards.
2. Adjusting your desk and monitor height
- Position your computer monitor to the height of your eye level and at least an arm’s length away to reduce any strain on your neck or eyes. A good height would mean you shouldn’t have to hunch over or tilt your head up to see the computer screen. If you are using a laptop, adjust the height by using a laptop stand when typing to reduce strain and tension.
3. Organizing your desk space
- Keep frequently used tools within close proximity to minimize reaching. For instance, keep your keyboard mouse, pen and notepad, and telephone nearby to avoid repeatedly twisting to reach for these things. Make sure that there is clearance under your desk for your knees, thighs, and feet and try to not store items under your desk.
4. Having good posture
- To reduce strain, ensure your shoulders are relaxed and placed back. Align your head with your shoulders, and keep your hands at or below elbow level. Continue to be aware of your head position and posture throughout the day, as we often forget about our posture from concentrating on the computer too long.
5. Taking regular breaks and stretching
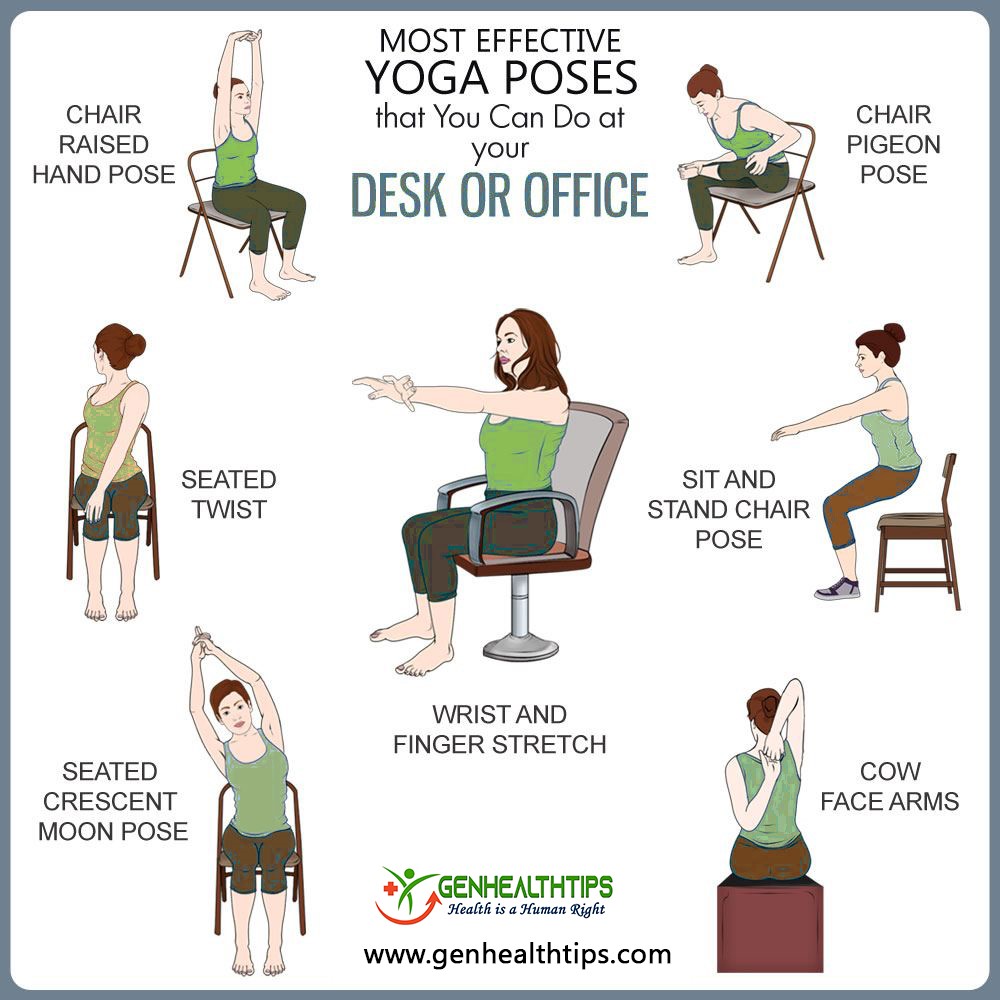
- Follow the 20-20-20 rule: After every 20 minutes of looking at your computer screen, give your eyes a 20 second break by looking at something else that is at least 20 feet away. Sitting at a desk for long periods of time can cause tight muscles and long-time compromise for pain in your back and neck. It’s crucial to remember to take stretching breaks every 30 minutes to relieve some tension and avoid pain overtime. Below are some stretches you can follow. Alongside with stretching, take a few minutes to go on a short walk to get your body moving and reduce eyestrain from starring at a computer for a long time.

Proper Lifting
Posted on October 3, 2020 by admin
Why is the proper lifting technique important?
One of the most common causes of lower back injury is incorrect lifting technique. When you lift an object with bad posture, this causes a greater load to be placed through the bones, ligaments and discs in your spine which may lead to injury. Remember to use the correct body mechanics to lift safely and prevent back injury.
Before you lift, make sure to consider the following:
- Know the weight of the object – determine whether you are able to lift it on your own.
- Get help if the load is too heavy to carry on your own.
- Make sure your lift pathway is clear (check if the floor is wet/slippery, remove tripping hazards).
Lifting steps:
- Stand close to the object you will be lifting.
- Keep a wide stance – your feet should be shoulder width apart with one foot being slightly in front of the other to keep balance.
- Squat down when picking up the object by bending your knees and keeping your back straight. Bending your knees reduces the load that is created in your lower back, which can prevent back injuries from occurring.
- Lift the object slowly by using your arm and leg muscles rather than your back muscles and straightening your hips and knees. Breathe out as you lift. Remember to keep your back straight and do not twist while lifting!
- Hold the object as close to your body as possible. Hold the object near your abdomen region – do not hold the object above shoulder level.
- Pivot your feed by taking small steps to change directions. Do not twist your body.
- Bend your knees while slowly and carefully lowering the object to the new location.
- Cervical stenosis: In this condition, the narrowing occurs in the part of the spine in your neck.
- Lumbar stenosis: In this condition, the narrowing occurs in the part of the spine in your lower back. This is the most common form of spinal stenosis.
- Numbness or tingling in a hand, arm, foot or leg
- Weakness in a hand, arm, foot or leg
- Problems with walking and balance
- Neck pain
- In severe cases, bowel or bladder dysfunction (urinary urgency and incontinence)
- Numbness or tingling in a foot or leg
- Weakness in a foot or leg
- Pain or cramping in one or both legs when you stand for long periods of time or when you walk, which usually eases when you bend forward or sit
- Back pain

Spinal Stenosis
Posted on August 21, 2020 by admin
What is spinal stenosis?
Spinal stenosis, or narrowing of the spinal canal, is a condition that can squeeze sensitive spinal nerves. Some people with spinal stenosis may not have symptoms. Others may experience pain, tingling, numbness and muscle weakness. Symptoms can worsen over time.
The most common cause of spinal stenosis is osteoarthritis, the gradual wear and tear that happens to your joints as you age over time. Spinal stenosis is common in older adults because osteoarthritis begins to cause changes in most people’s spines by age 50.
The two main types of spinal stenosis are:
Symptoms
Cervical spine (in the neck):
Lumbar spine (in the lower back):
How can chiropractic treatment help with spinal stenosis?
Chiropractic treatment is an all-natural, non-invasive method of helping relieve painful symptoms as well as addressing spinal stenosis directly at the source. Chiropractic approaches spinal stenosis holistically; taking into account your symptoms, the current state of your spine, how your body is feeling, what makes your symptoms better or worse, and what you feel comfortable doing.
To diagnose spinal stenosis, your chiropractor may ask you about signs and symptoms, discuss your medical history, and conduct a physical examination. Then, they may order several imaging tests to help pinpoint the cause of your signs and symptoms. Imaging tests include, X-rays, magnetic resonance imaging (MRI), or CT scan. Spinal manipulation and other manual adjustments are the primary method of treatment.
Chiropractic treatment aims to widen the space available for the spinal cord within the spinal canal. By correcting the displacement of spinal discs, relieving tension held in tight muscles, and removing the pressure from spinal nerves, a patient with spinal stenosis can experience lessened symptoms. Chiropractic care is drastically less invasive than other treatment options such as injections, harmful medications, or open spine surgery.
If you’ve been suffering from spinal stenosis in either the cervical, thoracic, or lumbar spine, or have felt symptoms that you believe can be spinal stenosis, contact us to book an appointment.
